According to Cancer Research UK, about 1 in 14 men and 1 in 19 women will be diagnosed with Bowel Cancer during their lifetime. For these people, being told it’s bowel cancer will be the start of a very difficult process. A process that not all of them will survive.
The good news is that, thanks to the ongoing improvements in treatment and care, more than half, 57%, of those diagnosed will survive. A number that continues to rise.
But for a lot of people, myself included, before there is a diagnosis, there are a series of steps leading to the point you find yourself being told it’s bowel cancer. Or, hopefully, told that it’s not bowel cancer.
Either way, each of these steps involves an growing amount of suspicion and fear that something is wrong with you. Each step involves another procedure that you don’t want to have, and, increasingly, seems to be heading toward one destination. Until, finally, you’re sitting in a room, with concerned looking health professionals, being told it’s bowel cancer.
This isn’t the same as a diagnosis, that comes next. This post is an account of how I found myself being told it’s bowel cancer.
Just to be clear, bowel cancer may also be known as colorectal cancer (CRC), or colon cancer. It’s all the same thing.
Bowel cancer has a number of recognised signs and symptoms and, in hindsight, I missed some of them. I’ll cover these symptoms in more detail in another post because they’re useful to know. But, for me, I didn’t think about them, or didn’t want to think about them, until far later than I should have.
One of the most obvious, and recognised, symptoms is blood in the stool. This one I was aware of, because my dad had been treated for bowel cancer some years before, and this was something he talked about. But, for him, blood in the stool was; BLOOD in the stool. There was no messing around or second guessing what was happening. For dad, one day he was on the toilet and boom! (or, more likely, splash!): blood everywhere. Dad went to the doctor, went to hospital, had surgery, made a full recovery. Didn’t even need chemotherapy.
That’s what happens when you catch it early. That wasn’t my experience.
But the thing about the blood in the stool symptom, is that the full wording is: “Blood in the stools without other piles (haemorrhoids) symptoms.”
Now, I’ve always been a big lad, which is code for, overweight. Which is, itself, often code for, fat. And, in the run up to my diagnosis in April 2014, I was very active. I was playing regular hockey at Taunton Vale. I was doing regular cycle rides into November 2013… at which point I got knocked off my bike and broke my collarbone, which ended that for a while.
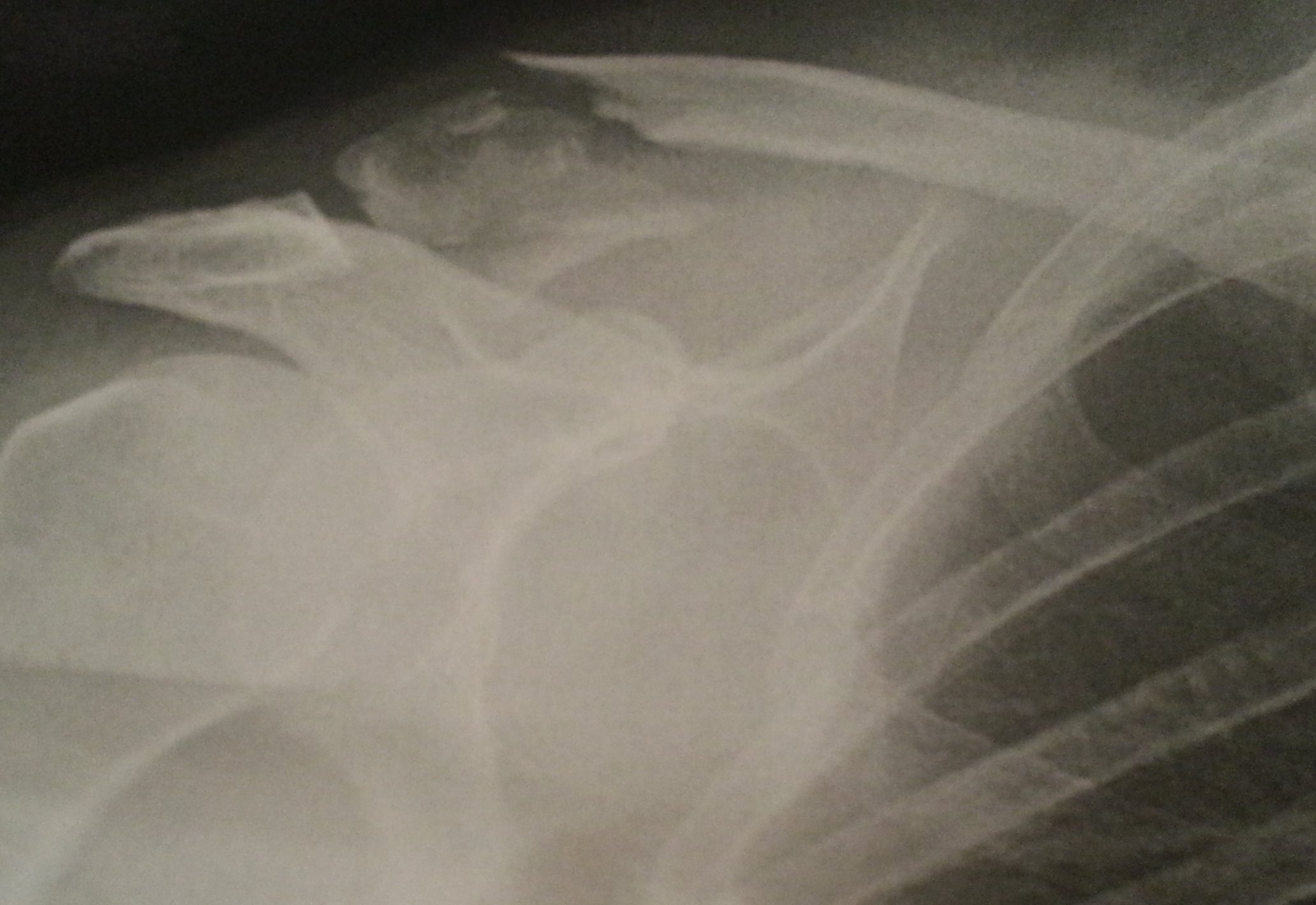
The point is, I was, ahem, overweight and exercising a lot, and sweating a lot and, let’s face it; piles were inevitable. So I was seeing a small amount of blood when going to the toilet, consistent with piles.
The thing is, though, and this is the really important bit: having piles does not mean you can’t also have bowel cancer. Especially, as it turned out for me, if the tumour is just round the corner, so to speak, in the rectosigmoid junction.
So, blood in the stool didn’t alert me. Nor did the increasing fatigue I was feeling during the hockey season. Every match was harder than the last until, at the end of the season, I could only manage 10 minutes before having to take a knee. Mid match. Repeatedly.
But this I wrote off as diet-related tiredness. I was in the midst of yet another diet and was being quite strict on what I was eating. Which meant I was running a calorie deficit, so of course I was getting tired…
Do you see the pattern developing here? In hindsight it’s obvious. At the time, the excuses seemed entirely plausible.
Seeing my GP
What finally drove me to see my GP was a change in bowel habit. And even that, I nearly wrote off as diet related. I won’t subject you to any more information about this change in bowel habit, other than to say it was noticeable and obvious.
In late January, I had an appointment booked with my GP because of a persistent cough. As the cough had nearly cleared up, by the day of the appointment, I nearly cancelled it. My wife, Julie, however, persuaded me to go and talk to the GP about my bowel issues instead. It’s safe to say that I wouldn’t be here, today, if she hadn’t talked me into going, because, by October, the tumour had grown so large it caused my bowel to rupture. And that was after three months of chemo!
So, I made myself go to the GP. And I didn’t want to go to the GP. Because the GP was going to stick his finger up my bum…
And that would be embarrassing!
The thing is; GPs are clever people. They must be clever people to pass all their exams. So, being clever people, they know there are going to be times they have to stick a finger up someone’s bum. It’s no big deal for them.
And yet I was seriously thinking about ignoring all the things happening to me. Writing them all off to diet issues and piles, rather then have someone stick their finger up my bum. Something they know and accept as part of their job.
Yeah, I know; I’m an idiot. Sadly, I suspect that I’m not alone. Please don’t be like me. If you’re in a position to advise someone in a similar situation to the one I was in, please encourage them not to be like me. Sooner is better.

When I arrived for my appointment, which was right at the end of the day, the surgery was running nearly an hour late. Which means, by the time I got to the GP I was already feeling awkward because he thought he was seeing me about a cough, and it was now so late. So I mentioned my change in bowel habit, suggesting it was related to diet and probably nothing. But he said otherwise and snapped on a rubber glove.
He didn’t really.
What he did was give me a rectal exam as described here. And it was nothing. I barely felt it and it was over in seconds. Nothing to worry about at all. Not that, the process of the exam was what I was worried about, I was embarrassed that he had to do it at all. Even this concern all but disappeared when it became clear he was simply following a protocol, probably laid out in a manual somewehere.
It was all very professional and far less embarrassing than I thought it would be.
Having done the examination he told me that it felt like haemorrhoids. He then drew some blood, to run some tests… just to be certain. And, while he was sure it was haemorrhoids, he’d call me back for a follow up appointment when the results were back.
I remain very grateful to my GP. If he hadn’t insisted on doing the examination; again, I don’t think I’d be here today. If he hadn’t, by the time I got round to defeating my reluctance to go back, it would’ve been too late to give me a fighting chance.
After the appointment, I was relieved to hear that the doc was sure it was haemorrhoids. I accepted this completely, although I was a little suspicious about the need for a blood test. Julie started worrying.
I was called back to see the GP a few days later, and he said that the results of the blood tests were unusual. My haemoglobin levels were a little low, at 11.7, but my Ferritin levels were very low, at less than 5. Together, these indicated that I’d been likely been losing blood for a while.
The doc said that; while he was still sure it was only haemorrhoids, he was going to refer me to the hospital for a rigid sigmoidoscopy. It was part of an accelerated process that guaranteed I’d be seen within two weeks. This wasn’t me being told it’s bowel cancer, this was me being told to not worry because it probably wasn’t bowel cancer. Looking back, this was me being managed, so as to avoid panic. And it worked. For me. Julie was starting to get very worried.
Rigid Sigmoidoscopy
The rigid sigmoidoscopy was done at the hospital and the process was very similar to that of the digital examination done by the GP. Except this time there was more paperwork involved, and I had to change into a gown first.
I saw the rigid sigmoidoscope, as I was arranging myself on the examination bed. It was just a fairly thin, straight tube, connected to some wires.

The sharp eyed will notice there is also a bellows. I didn’t at the time. And that came as a shock, I can tell you. The ‘scope going in was neither here nor there, although it was a bit cold. Being inflated, on the other hand, was a very strange sensation.
The air goes in to make room for the ‘scope to ‘see’. It has a light and a video feed going back to either the user or a monitor. The air, however, isn’t removed afterwards, leaving a bloated feeling and the fear you’re going to fart, uncontrollably, at any second. I didn’t, though, so no need for concern.
After the procedure, I was told that the examination was inconclusive and that I’d need a colonscopy, which would be booked in for me. Since 2014, when I had my rigid sigmoidoscopy, most of these procedures are now done with a flexible sigmoidoscope. It’s the same idea, except that the end of the ‘scope can look round corners. Which, in my case, would have been very useful.
After only a few days I got the report from the rigid sigmoidoscopy examination. The report included such reassuring phrases as, ‘no palpable masses’ and, ‘no supraclavicular lymphadenopathy’. I had no idea what that second one was, but there was none of it, which I took to be a good thing.
Then the report went and spoiled it all by stating there was, ‘blood in the rectum above the haemorrhoid levels.’ Not piles then!
While this was still not us being told it’s bowel cancer, frankly, the alternatives were running out. Julie, by this time, had accepted it was bowel cancer. I decided that it couldn’t be cancer and was most likely Ulcerative Colitis.
Colonoscopy
I got the paperwork through that told me that my colonoscopy was booked for the 21st March. And, unlike the rigid sigmoidoscopy, where there was no form of internal rinsing, for the colonoscopy, no chances were being taken: they wanted that bowel to be clean!

With the appointment letter came a Patient Information booklet, a diet sheet and a pack of medication. The booklet explained everything to expect and the diet sheet included details of how to maintain a low residue diet in the days before the procedure. This diet was effectively right up my street as it meant no fruit and veg but plenty of bread, rice, pasta and, I kid you not, sponge cakes.
Sadly, this joyful diet was short lived and was effectively counteracted by what the medication did to me. I was given moviprep. Moviprep is not your friend. Basically, you make yourself a huge, not particularly nice tasting drink, and then drink it over a couple of hours. Wait a short while… and then the world falls out of your bottom.
Then, do it again!
Depending on when your procedure is booked, you’ll either drink one Moviprep at night and the other in the morning. Or you’ll drink both in the same evening. At the same time as drinking the Moviprep, and for a full 24 hours before, there is fasting. The one good thing about Moviprep is you don’t feel hungry after it’s finished with you.

At the hospital, before your procedure, there is an interview with a nurse. This is to make sure you’re ready and to see whether you’d prefer a light sedation or Entonox, more commonly known as, ‘gas and air’. Or you can choose to have both. Or neither.
I went for Entonox because if you have the sedative, you can’t drive for 24 hours. And I had a hockey match the following day! So, I filled in the paperwork, said goodbye to Julie, and was taken through to the ward. I was shown to my bed and asked to change into a gown.
From there we walked down to the procedure room, and I was introduced to the consultant doing the procedure. At this point I saw the colonoscope for the first time. It was somewhat more imposing than the rigid sigmoidoscope…
But then I was asked to lay on the bed, on my left side, with my knees drawn up. I took a couple of deep breaths on the Entonox, and we were away.
Almost immediately, I discovered than I don’t get on with Entonox, which was fine, because a few seconds later, I heard a grunt of surprise from the consultant. I looked at the screen and the view form the camera was completely obstructed by what looked like white frond structures. A lot like seaweed, but white.
Now, I’m no doctor, but I’d done a bit of biology in my time and I’d seen every episode of House M.D., so I knew something wasn’t right. I tried to speak but the Entonox was messing me up, so I stopped breathing that and started talking to the consultant.
The consultant seemed somewhat surprised by this turn of events but, after a bit of persuading, was willing to answer my questions. I very quickly learned that asking things like, ‘is that cancer?’ got responses like, ‘we won’t know until we get the results of the biopsies.’
Whereas asking, ‘in your experience, would you say that was likely to be cancer?’, got a straight answer.
The answer was, ‘yes.’
I was finally being told it’s bowel cancer.
After being told it’s bowel cancer, much of the rest of the procedure passed in something of a blur. It was a lot to get my head around, because I’d still been telling myself it was Ulcerative Colitis. But, to be honest, the distraction was a blessing, because the procedure was very uncomfortable.
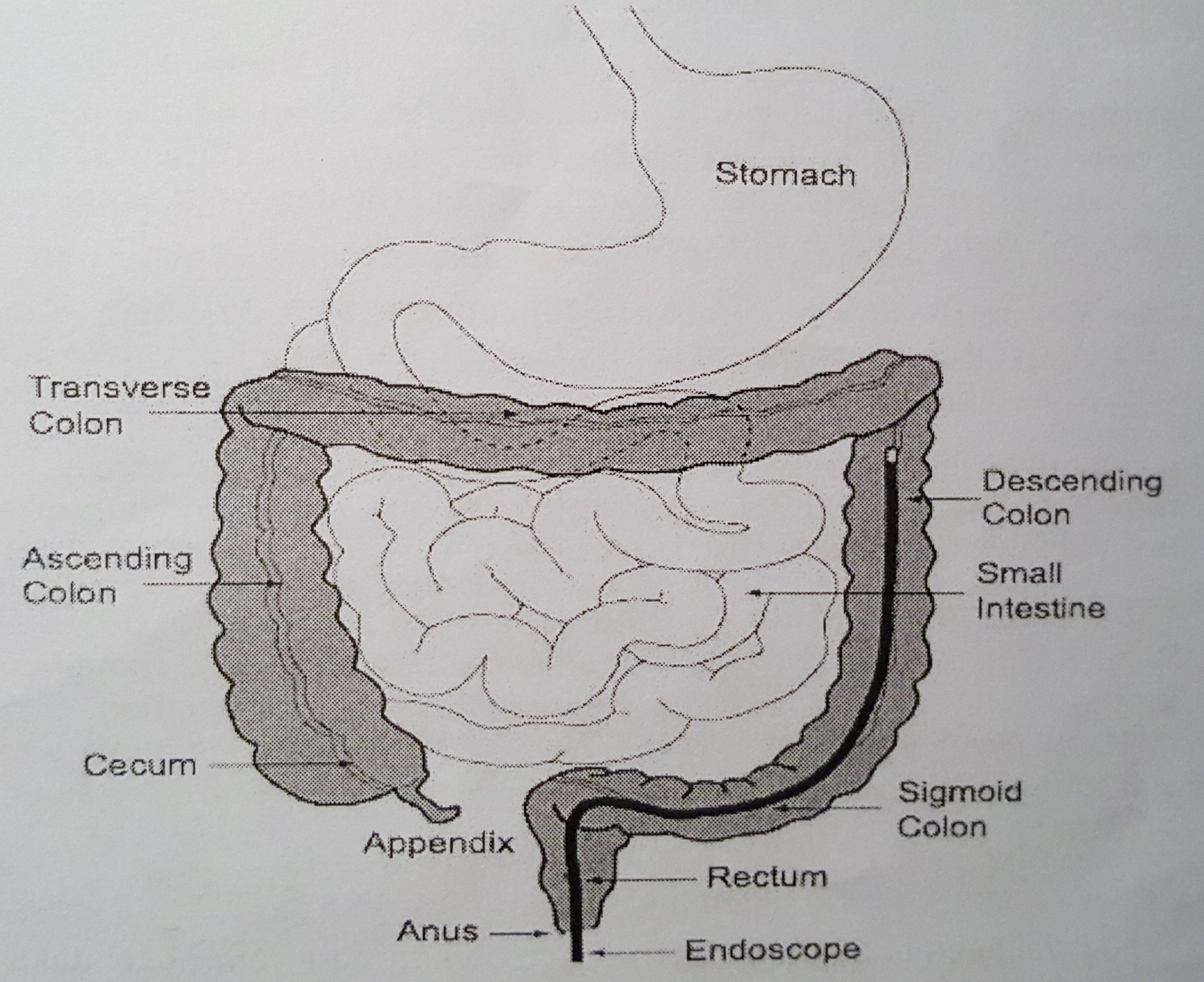
The issue, again, was the air. The colonoscope also had an air hose and the consultant seemed to have set it on, ‘inflate dirigible’ mode. A lot of the problem was that the consultant wanted me to relax my bum. But that would’ve effectively meant I was more or less farting in his face. 40 years of fighting the urge to fart in public is difficult to overcome on command. The other, more practical, problem was that there was a lot of tumour to get through, so he was having to work hard to get the ‘scope all the way in. And introducing more air, to ease the grip on the ‘scope, seemed to be the answer.
It was an uncomfortable experience. Which is why, when I had my next colonoscopy, I chose the sedative option. And, you know what? No problem at all. My advice is: always go with the sedative.
In the end, the consultant got all the way round to the appendix and headed back out again, deflating as he went. He paused to take a bunch of samples from the cancer fronds and then we were done. I was wheeled back to the ward and allowed to clean up, while one of the nurses texted Julie to let her know we were ready for the meeting.
I was still feeling very bloated by the time we sat down for the meeting. A feeling that lasted well into the night. Seriously, choose the sedative and feel much more comfortable. The effects of the sedative pass quickly enough that you’ll be alert for this meeting.
The meeting was tough. Everyone in the room knew Julie and I were being told it’s bowel cancer, except for Julie. As it was, when the bomb dropped, Julie took it very well. She said, later, that she’d worked out that it was going to be a cancer diagnosis some time ago, and was waiting for me to accept it.
Being told it’s bowel cancer was a tough thing to hear. But the colorectal staff were amazingly professional and supportive. They still are.
But, being told it’s bowel cancer, isn’t the same as a proper diagnosis of bowel cancer. For that, you need the results of the biopsies and at least one scan to discern the extent of the problem. A process I’ll cover next time.
8 thoughts on “Being Told It’s Bowel Cancer”
Oh my god I just think you are both such incredible people dealing so positively with what is an horrific disease. And all praise to you Paul for trying to ease people’s journeys on the road to diagnosis.
Fantastic blog..
Hi Ang,
Thanks again.
As you can probably tell, I’ve finally worked out how to respond to comments… Tricky things, websites.
Paul
Thank you so much for sharing this experience as I am at the beginning of this journey hoping it is either piles or colitis.
Hi Sheila,
Sorry for the delay in responding, I’ve been struggling with my mindset for a while and haven’t been on here.
I’ve got my fingers crossed for piles (which is a sentence I never thought I’d find myself writing…!). If it’s anything else, and you’d like to talk things through (or anything else, really), please let me know and I’ll help in any way I can.
I wish you well,
Paul
I’m so glad I stumbled across your page. It was very well written and gives me a better insight on my mom and aunt who were both diagnosed with colon cancer. I also have been bleeding for over two years now but they keep saying all is well. So I hope “they” know what they are talking about. This makes me want to go get checked yet again as I don’t want to be told stage four when it could be stage one. I wish you well and may God bless you and your family. Deborah
Hi Deborah,
I’m very happy that you found my page helpful.
Sorry to hear that your mom and aunt are having to go through this as well. If you’ve been bleeding for two years and haven’t had a colonoscopy, I’d suggest that it might be worth having one done. If you’ve had one, and it was clear, then my understanding is that all should be well. That said, I completely agree with you that it’s worth keeping on top of. Better, I think, to be overcautious than to miss something. Hopefully, though, you’ll live a long and cancer-free life.
Best wishes to you and yours,
Paul
Hi
Thank you for sharing,I am from India,an old patient of Ulcerative colitis,just 3 days back after colonoscopy I was told ,I have a bowel cancer. I was not shattered rather confused, your blog is clearing a lot of doubts , and I am feeling very confident to face the future.
Hi Parag,
I’m really sorry to hear your news, but very glad that you are so positive for your future.
If I can help at all, please let me know.
Best wishes for your improved health,
Paul