Liver surgery for bowel cancer is a strange concept to get your head around. Stranger, still, in my case, was the decision to do the surgery on the secondary tumours on my liver before the primary tumour in my bowel.
I wasn’t involved in the decision making process for this, I was simply informed that this was the route that would be taken. The decision is seemingly made by some sort of committee. This committee may well be comprised of the surgeons and oncologist directly involved in my case, I just don’t know. What I do know is that somewhere, an agreement was reached to do liver first and then bowel.
As you can probably guess, this would not have been my choice. It wasn’t the choice of the surgeon who would be removing my bowel tumour, either; I know that much.
I understand the reasoning behind the decision. The liver surgery was smaller and would involve a shorter recovery time, thus allowing both surgeries to be completed as quickly as possible.
My view, though, was that the bowel tumour was spitting out metastases and I wanted that stopped before it could do any more. I wanted the bowel surgery for bowel cancer before the liver surgery for bowel cancer; it just made sense. But the medical professionals had spoken and I accepted that they were the experts, so theirs was the way forward.
Before my surgeries, and having survived the complications of chemo session 2, I had to get through the side effects of chemo sessions 3 and 4. After 4 sessions in 3 months, the biggest, most obvious side effect of the course of chemotherapy, was my belly. I put on 2 stone in that time.
Worse than the weight issue was what the follow-up scans showed. There had been no shrinkage of my tumours. Very far from ideal. But, while the scans didn’t show a change, I felt one. It was somewhat easier to go to the toilet than it had been, so there must have been some reduction in the bowel tumour. I was told that the lack of shrinkage wasn’t a major concern, though; the main aim of the chemo was to kill off any small tumours that were trying to set up shop elsewhere in my body. That made the news more palatable.
In the South West of England, different hospitals have different specialties. The local hospital in Taunton, Musgrove Park, did a roaring trade in bowel surgeries but was not set up for liver operations. For that, I needed to go to the Bristol Royal Infirmary (BRI).
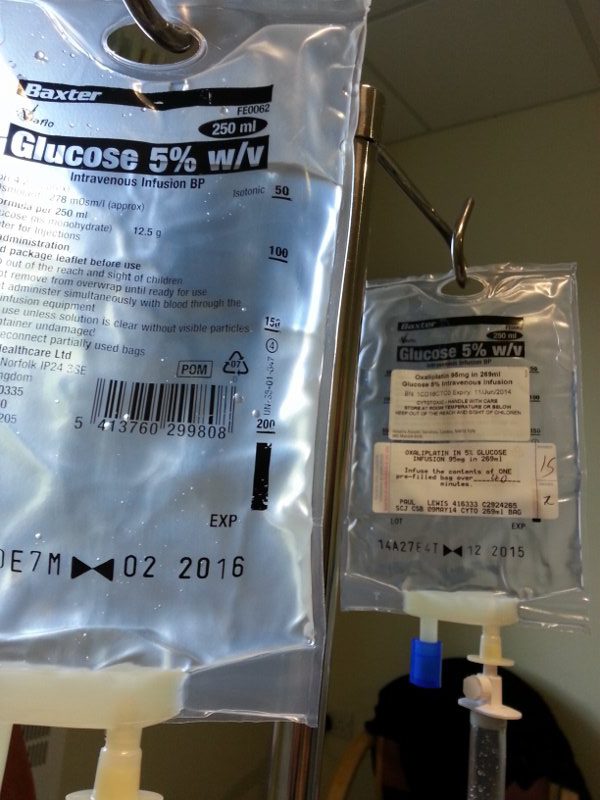
In the meeting with the consultant liver surgeon at the BRI, I was told that the scans showed my gallbladder to be full of gallstones. Before I got a chance to digest this, I was told that it wouldn’t be a problem because one of the tumours was right next to the gallbladder, so it would be removed during the surgery. So, that was it, the surgery was on. Happy days.
Before I could have the liver surgery for bowel cancer, I had to attend the hospital for a preoperative assessment. I was sent a date and a questionnaire to complete prior to said date. There wasn’t time to post it back, so I took it with me, where it was promptly ignored and the nurse worked through a subtly different one.
I was weighed and measured and an ECG was done. Then swabs were taken of my nose and then groin, to check for MRSA. But, because the swabs wouldn’t be analysed in time, I was then given a shampoo and a cream and a schedule of their use. The shampoo was fine. The cream, however, was for my nose, and I had to apply the cream to the inside of my nose a couple of times a day. I did as Instructed. As it turned out, I didn’t have MRSA anyway.
And, a few days after the preoperative assessment, and only 10 days after meeting the consultant, I was back in Bristol for my liver surgery for bowel cancer:
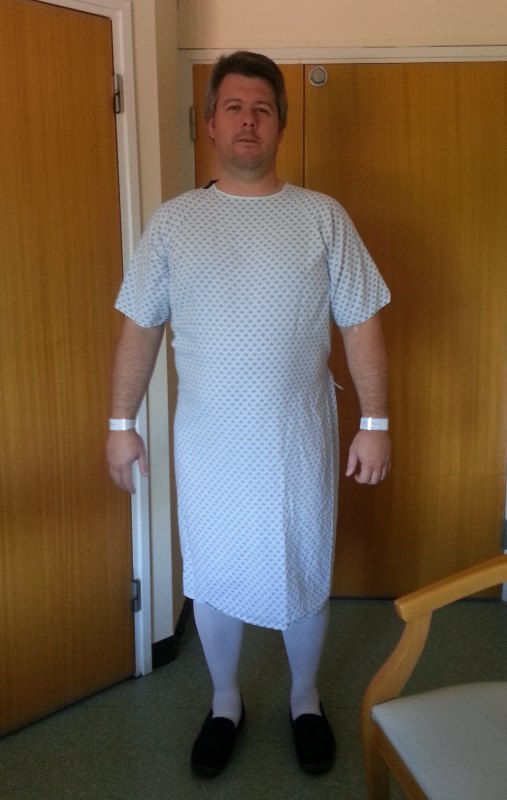
My liver surgery for bowel cancer was to be done laparoscopically, through keyhole surgery, and is known as a resection. The idea is to completely remove the tumour as well as a margin of healthy tissue, to ensure it is all gone. In my case, the margin included part of the gallbladder, so the whole thing had to go.
Laparoscopic liver surgery for bowel cancer is done under general anaesthetic, which means there’s always the slight chance you won’t wake up. A 1-2% chance, in this instance. It also means a stay in hospital is required, first in the Intensive Care Unit, then the High Dependency Unit, then in a ward for at least a couple of nights.
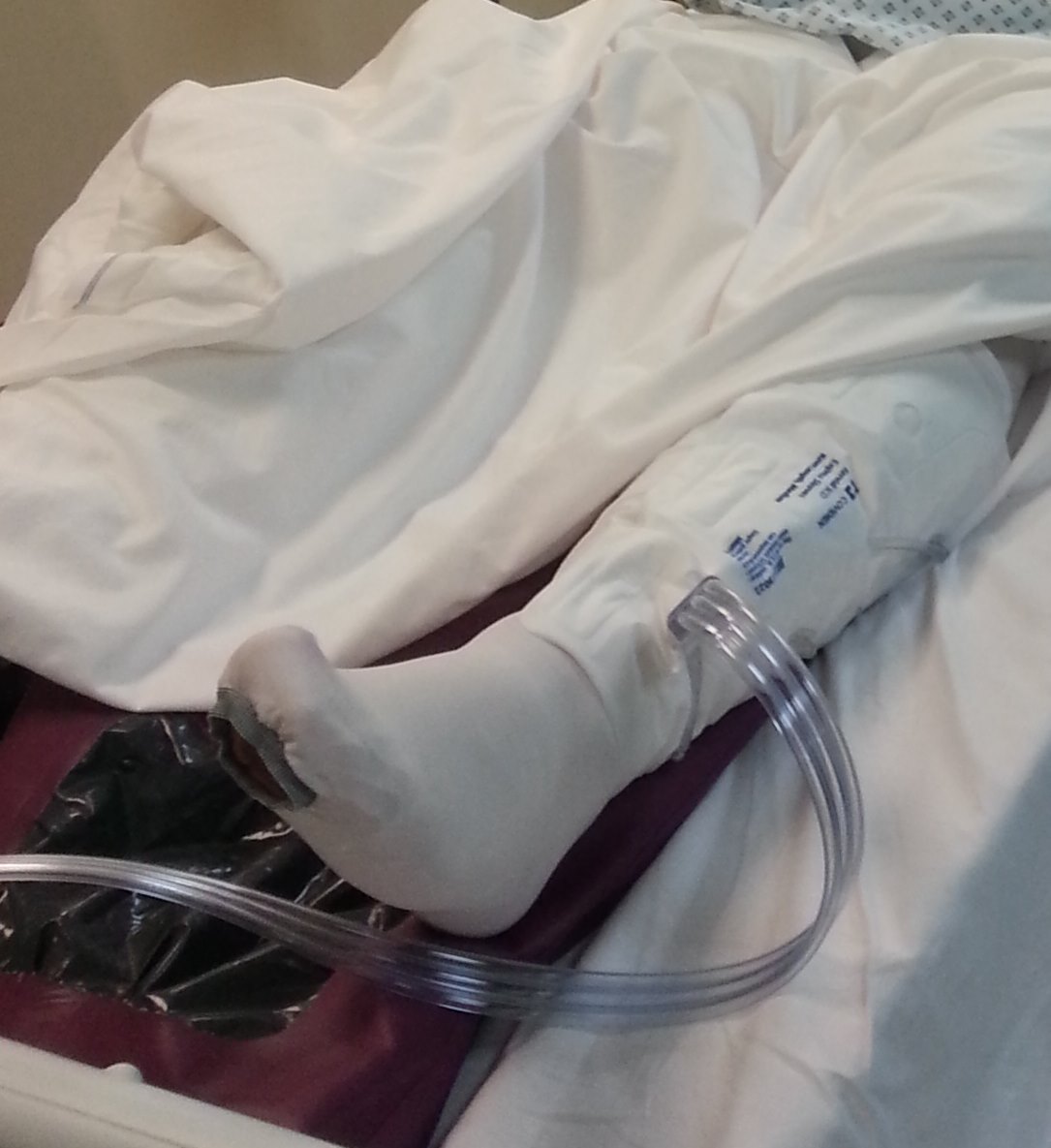
All this means that you’re never quite sure what’s going to have been done to you while you were out. When I woke up, I looked like this:
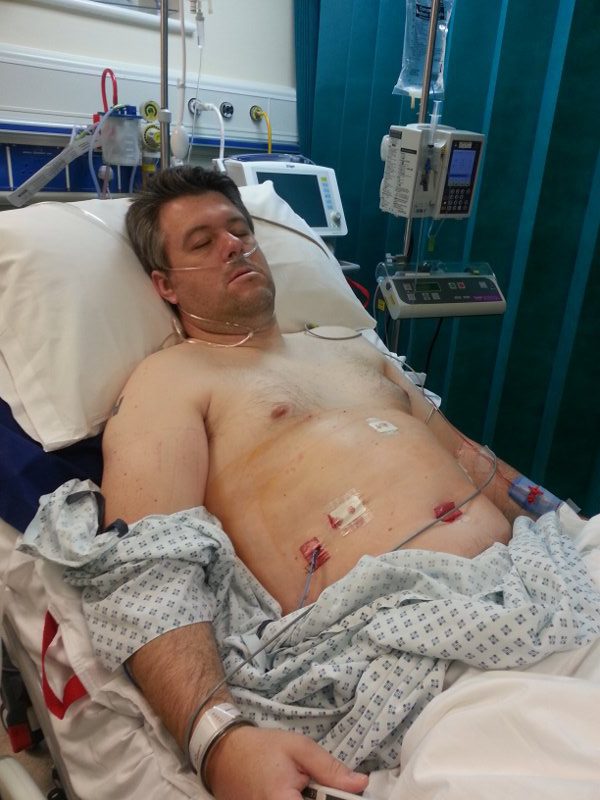
Not including the needles, the liver surgery for bowel cancer left me with 5 new holes. Including one in my belly button… what sort of monster hacks their way in through your belly button?! Not that it made any difference, in the long run, in a couple of surgery’s time, my belly button would be removed completely. Still, it was nice of the surgeon to attempt to limit the number of visible scars.
The focus of this liver surgery for bowel cancer was the right side of my liver. You can see that there’s still a drain in place at this point. I’m also on oxygen because my low heart rate leaves my blood oxygen levels sufficiently low to freak out anyone that sees them. I quite like being on the oxygen but it really dries my nose out.
The main thing was that I survived. And that the liver surgery for bowel cancer was a success. Tumours removed with good, clear margins. Everyone’s a winner.
The actual process of keyhole surgery is a bit strange the first time you hear about it. The 5 new holes were all to allow access for a piece of surgical equipment. One of the pieces of equipment is a glorified air pump. The patient is effectively inflated. This is to create the space needed to access the cancerous parts of the liver. Other pieces of equipment include the light, the camera and the means to carry out the action: a cutting or a burning tool. Anything that is cut away, then needs to be removed from the cavity, which requires another item of equipment…
But lots of small incisions are much quicker and easier to heal from, than one large incision. The main problem with this technique is the inflation aspect and the air that’s left behind. Not just that you’re left bloated by the excess air, although you are. No, the main issue is the referred pain.
The gas used to inflate the abdomen is CO2. Some of this will get left inside you. On the first day after surgery, while you’re lying down, this isn’t a problem. Thereafter, when you start sitting, standing and walking, the CO2 rises up and forms bubbles under the diaphragm. The gas irritates the diaphragm and, because the same nerve serves the diaphragm and the shoulder, it is often the shoulder that gets told it’s in pain. It isn’t, nowhere is actually in pain. But that doesn’t stop the shoulder from telling the brain it’s really suffering.
It happens for about 70% of people. Including me. It passes after a couple of days, when the CO2 dissolves into the body. But boy, does it hurt in the meantime!

The best way to ease the pain is to lie down again. But medical staff don’t want to see that, they want to see you sitting, standing and walking, because that’s the best road to a speedy recovery. And, when you mention it, all they’ll say is that it’s nothing to worry about and that it’ll pass in a couple of days. All true, of course, but not hugely helpful. What is helpful, is that the shoulder pain actually distracts from the surgical wounds and allows you to move around more easily.
But, before you have to worry about the shoulder pain, you have the first day in recovery. You will be expected to sit out of bed on the same day of the operation, if it’s a morning surgery. And early the next morning, if it’s an afternoon surgery. The biggest handicap to sitting out of bed is all the things attached to you.
After this surgery, I didn’t have a urinary catheter, so at least I didn’t have to worry about that. And worry you do. No matter who you are, you don’t want the catheter to get snagged on anything…
You won’t be expected to move to the chair on your own, there will be at least one nurse helping you. The simplest thing is to do exactly what you’re told and to move sloooooowly. If you don’t have a catheter, as I didn’t, around this point you’ll be given a cardboard urine bottle and asked to fill it. Because you’ll have received intravenous fluids during your operation, literally filling it might be an option. You may well still be receiving IV fluids at the point you’re filling the bottle. They’ll want to measure your output, so don’t drop it.
You may also get offered a bed bath, during this time. I was suitably bored by that stage so agreed to have one. Yeah, never again. No matter how awkward you think it could possibly be, it’s much more awkward than that. Better to hang on a day and have a shower. The nursing staff will want to see you independently shower before they let you go, anyway.
The first night is very far from a peaceful experience. I had inflating stockings on my lower legs. These things inflated and deflated about twice a minute… all through the night. In addition to that, there is a requirement to take very frequent observations of blood pressure, heart rate and blood oxygen. This may require you to have a sphygmomanometer cuff around one arm, which will inflate at regular intervals. There will likely also be a clip on a finger for the blood oxygen.
If the clip is dislodged, alarms go off. Or if your heart rate goes too low, alarms go off. And if your blood oxygen gets too low, alarms go off. Also, if you’re in a room with anyone else, their alarms can go off. The cuff on your arm keeps inflating. The stockings on your legs keep inflating. And, as a bonus, someone will come round every now and again to check your temperature. Sleep is tough to come by.
Besides showering, before you can go, you’ll need to, ‘open your bowels’. The experience of a succession of nurses starting their shift with the question, ‘have you opened your bowels yet?’ is difficult to put in words. As is how you’re supposed to answer when it’s finally happened. Although, “Hell, yeah! High five?”, is definitely to be avoided.
The reason for the interest is that abdominal surgery, even keyhole liver surgery for bowel cancer, can stall the digestive system. Until they know that it’s working properly, the nurses can’t be sure there isn’t a problem. So you won’t be allowed to leave.
Over the course of the first day or so, bits that have been attached to you get removed. The oxygen will go after the first night. The catheter, if you have one, at some point during that day. The number of cannulas in your hands and arms will drop to one on that day, and zero after the second night, providing all is going well. It’s better to have easy access for IV fluids and medication until there’s no chance of complications.
Usually the last thing to go is the drain. My drain stayed in a couple of days and only collected a very small amount of liquid. So, after the second night, it was removed and I was free to go home.
By then, I’d ticked all the necessary boxes in the toilet. I’d had a shower. And I’d been seen by the physio, who had walked me up and down a couple of flights of stairs. The actual removal of the drain was an unpleasant experience, I think because I could feel the suction as it was removed. I didn’t like it. I’ve never had that experience in any of my surgeries since, so it’s nothing to worry about. But follow the instructions of the nurse, when it’s being removed, just in case.
By this stage, my pain medication was down to paracetamol; two tablets, four times a day. It still seems strange thinking that such light medication was able to do the job, but it was.
So all I really needed to know, before I could leave, was how to look after myself. A nurse changed the dressings, just before I left. She applied a couple of butterfly stitched to the drain site, because that was still open from the removal of the drain. Then some clean waterproof dressings went on and I was given two more sets of the same dressings for when I was at home. I was told to make sure I kept the wounds dressed for at least a week, then she moved on to my feet.
Well, my lower legs, really. I still had compression stockings on, to prevent a deep vein thrombosis. I was given a spare, clean pair of stockings and told to keep wearing them until I was moving around normally again.
And that was it. Two nights after my liver surgery for bowel cancer, I was off home. Amazing!
What was even more amazing is that I would shortly hear that my bowel resection surgery would be scheduled for just 15 days later.
Of course, it didn’t work out that way; there were… complications!